A collection of scientific studies, including "just stop the superspreading events" which appeared in The New York Times on 2 June, all demonstrating that the prevention of such events can slow the spread of COVID-19; an approach with much fewer social and economic consequences.
Lees volledig artikel: The big impact of superspreading events
The big impact of superspreading events
On June 2nd, the New York Times published an article called “Just stop the superspreading events”, which is completely in line with my findings from April about the great impact of superspreading events and that Covid-19 is actually spreading slowly outside those events.
These are the most important findings of the epidemiologists Adam and Cowling regarding the Covid-19 outbreak in Hong Kong. They investigated 1,038 infections in Hong Kong between January 23rd and April 28th and reported their results in this paper.
Their conclusions on 349 infections (the remaining 689 were infected elsewhere in China):
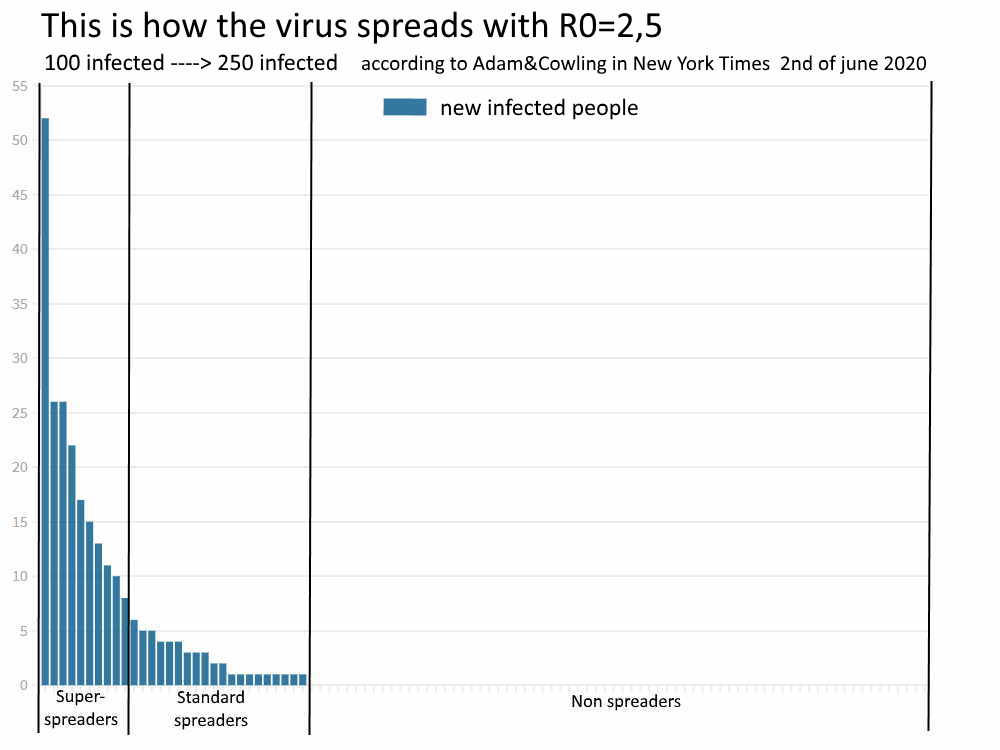
- 20% of those infected accounted for 80% of new infections. They all took place at social gatherings.
- 10% accounted for the remaining 20%. This meant that 1 or 2 people were infected, usually within the household.
- 70% of the infected persons, did not infect anyone else. The authors found this to be an astonishing outcome.
In addition, they mentioned other studies with more or less comparable results:
- The study in the province of Shenzen came to the conclusion that 80% of the infections were caused by 8 to 9% of the infected people.
- In Israel, a study found that 80% of the cases were due to less than 10% of all infected persons.
- In the case of SARS in Singapore it was found that 6% of the cases were responsible for 80% of the infections. 73% of the persons infected did not infect anyone.
- In Hong Kong, 331 SARS infections could be traced back to one person.
- For MERS in 2012 in Saudi Arabia, 14% of the cases accounted for 80% of the cases.
Not only they conclude that these superspreading events are part of the spread of COVID-19, but that they are the principal driving force behind the pandemic as well!
This is a selection of blogs where I came to the same conclusion:
– April 9: That’s how big the impact of superspreading events is
– April 19: Kessel’s superspreading event on 5 March
– April 24: The spread of the virus is already virtually under control
– May 1: Meat processing industry: superspreading hot spots
– May 28: COVID-19 doesn’t spread that easily at all
Patterns
Through research in Dutch municipalities where superspreading events did and did not take place before the Lockdown on 15 March, the same patterns can be seen as described by the two authors in the New York Times. Municipalities where a superspreading event had taken place, had on average a factor of 8 times as many infections and deaths as those where such an event had not taken place.
The final conclusion of the authors in the New York Times is that by preventing superspreading events, the spread of Covid-19 can be controlled. And they conclude: this can be done with an approach that has much less impact, socially and economically, than the lockdowns and the extreme form of social distancing that has been imposed on the world in recent months.
Their final sentence is: Forget about maintaining or reinstating drastic measures to control the spread of the virus in the event of new outbreaks. Focus only on stopping the super spread.
1.5 meter society
Although they don’t use the same name, they indicate that stopping the spread of the virus should not be done through a 1.5 meter society, but with measures to prevent the super spread.
The interview with Japanese professor Oshitami shows exactly the same. He is a member of the Japanese Intervention Cluster Group. This is the translation of the most important part:
“That fact not only made the contact research very inefficient, it was reminiscent of that other coronavirus from 2003: SARS. “That differs in many areas from Sars-CoV2, says Oshitani,” but SARS also turned out to be dependent on super-spreading events for its survival, with one person infecting many people at once and creating a cluster. “
Those clusters, the Japanese concluded, are key in tackling the virus. Oshitani was a member of the Cluster Intervention Group set up on February 25 by the Ministry of Health. The ministry changed the strategy of contact research by the Japanese GGDs: the focus was no longer on identifying and quarantining the contacts that a person who tested positive could have infected, but on finding out where this person had the infection. – what the Japanese call retrospective contact research.
Was not sick
For example, they identified one cluster after another, including in gyms, conference centers, restaurants, and karaoke bars – nearly all of them where people without masks gathered and talked or sang loudly. Also striking: the person who infected the others was not sick at the time and did not cough or sneeze.
‘This is how we came to our policy based on the three Cs: avoid closed (closed) spaces with poor ventilation, busy (crowded) places and intensive (close) contact such as close conversations,’ says Oshitani, ‘supplemented later by avoiding together. sing, talk loudly and make close efforts. “
The key to reducing the number of infections is not in applying the 1.5 meter society, but in ensuring that superspreading events do not happen!
But it means a lot more
One subject they don’t discuss in more detail in their article, is how the infection actually takes place. However, they do indicate that it takes place in enclosed spaces inside, with a lot of people present. But they do not express themselves about the method of transmission, via direct contact (as WHO/RIVM claim) or by air. These research results, partly thanks to statements by the OMT in the Netherlands and people like Prof. Voss, give a very clear answer. The OMT’s advice states the following as an argument that Covid-19 does not go by air: The reproduction number of Covid-19 is around 2.5. And then the OMT states:
“Virus diseases like measles, which are spread aerogenic through fine small droplets, have a much higher reproduction rate, between 12 and 20.”
In other words: Only if a lot of people are infected at the same time, this is evidence of small droplets floating in the air.
Let’s make some calculations based on the results of the New York Times article.
- The R0 of Covid-19 is 2.5. So that means that 1,000 people infect 2,500 other people.
- If 10% of the people infect 80% of the people, it means that (10% of 1,000=) 100 people infect (80% of 2,500=) 2,000 people. Then the R0 of this group is 2,000/100 = 20.
- If the remaining 90% infects the remaining 20%, 900 people still infect 500. Then the R0 of this group is 500/900= 0.6
R0
The high R0 of the first group (1 person infects 20 others on average) strongly resembles that of measles. So then the only logical conclusion you can draw as OMT and Prof. Voss, is that in superspreading events the spread is by air and not by direct contact.
The Robert Koch Institute now also indicates that airborne contamination does take place (chapter 1, section on aerosoles, last paragraph):
“Even if a final assessment is currently difficult, the studies so far generally indicate that SARS-CoV-2 viruses can also be transmitted through aerosols in the social environment.”
In super-spreading events, where many are infected at the same time, it could hardly have happened otherwise than by air.
You need a lot of fantasy and a lack of logical thinking if you want to explain the contamination of 52 people by one other member of Seattle’s choir by transmission through direct contact. If you accept that with the measles (R0 between 12 and 18) the virus spreads by air, then you can’t draw any other conclusion that Covid-19 does the same with those superspreading events.
So that way we can conclude that 80% of all COVID-19 infections are airborne.
Also with Influenza there are studies from the past, which are about the airborne spread of the virus. Such as this study from 2013 with the title “Aerosol transmission is an important mode of influenza-A spread”.
The question remains however, how does this infection occurs in the remaining 20%? Are these mainly infections within the household because of direct contact?
But if the infection is airborne at superspreading events, why shouldn’t it be the same within the household?
The answer to this appears to be given by the important results of Prof. Streeck’s study in Heinsberg. If you are infected during a superspreading event, you are more seriously ill and have fewer symptoms than at home.
Long-term exposure to the virus in the air is the crux of the matter. From the lungs of an infected person the virus ends up in the lungs of not yet infected people. Not only do they breathe the minimum amount needed to become infected, but many people present breathe in a lot of virus (high viral load) and become quite sick from it.
Floating
At home the conditions for the virus are apparently less favorable to strike that way. There may be more ventilation. The patient talks less and certainly doesn’t sing. The not yet infected persons do not stay in a room with the floating virus long enough to get sick of it. That’s probably why the researchers in Hong Kong establish that 70% of the infected persons have not infected anyone else at home.
Airborne infection also explains why people are not infected when there is good ventilation. And why there are hardly any infections in the open air. Then the virus doesn’t float around a person long enough to breathe in enough virus and get sick of it. That’s why higher humidity works, because it prevents the virus from floating around for a long time. That’s why mouth protection works in indoor areas, because it considerably reduces the emission of virus particles that remain in the air for a long time.
This also means that contamination via direct contact plays virtually no role in the spread of Covid-19. The measure that really worked all over the world is the ban on meetings with larger groups of people. And not the fact that we have introduced social distancing (keeping the 1.5 meter distance in the Netherlands). These are also the conclusions of researchers from Hong Kong.
Unsafe situation
As long as the WHO and RIVM do not recognize this, we will not only keep the stranglehold of the 1.5 meter society around the neck of the economy and social structure, but we will also maintain a fundamentally unsafe situation. As a result, based on RIVM’s protocols, we are doing exactly what is (virtually) ineffective in preventing the spread of the disease and are gradually doing what increases the risk of superspreading events. (allowing meetings with people, without pointing out the need for good ventilation).
It is similar to the situation where you drive down a single track on an unguarded level crossing. The RIVM’s track says that you only have to look to the left in order not to be hit by a train. You do exactly that. You stop in front of the crossing and look carefully to the left. And you don’t see anything coming, so you cross.
But then you are hit by the train coming from the right. It wasn’t in the RIVM’s track book, because that was the timetable from 2019.
You have just read: The big impact of superspreading events.
Volg Maurice de Hond op Twitter | Facebook | LinkedIn | YouTube.