This is how the spread of COVID-19 generally takes place I studied to become a social geographer. My specialty was research & statistics. In 1965 I learned how to program and have since always used computers intensively for my work. In huge crises like the one caused by the COVID-19 outbreak it is of major […]
Lees volledig artikel: This is how the spread of COVID-19 generally takes place
This is how the spread of COVID-19 generally takes place
I studied to become a social geographer. My specialty was research & statistics. In 1965 I learned how to program and have since always used computers intensively for my work.
In huge crises like the one caused by the COVID-19 outbreak it is of major importance to use a multidisciplinary approach. That explains my effort and approach.
For the past two months I’ve been studying the geographical patterns of outbreak the virus on a global scale. In doing so I used both old and very recent scientific studies to find answers to the following questions.
My questions
- Why were the first big outbreaks in Wuhan, Daegu, Teheran, Bergamo, Madrid, Brabant and Seattle?
- Why is the number of deaths in Lombardy higher than the total deaths in Africa and Latin-America combined?
- Why does Japan have 1 death for every million citizens, and the Netherlands 160?
- Why is the number of deaths in New York City 15 times higher per million citizens than San Francisco’s?
- Despite weeks of pointing out the risks for refugee camps, townships and favela’s, how come we see no big outbreaks in these places?
- no big outbreaks in refugee camps, townships and favelas
- What’s so special about the outbreaks in New Orleans and the coastal town Guayaquil (Ecuador)?
- How come so many people get infected and die in nursing homes?
- What explains the decrease in number of new infections in the Netherlands?
Coincidence is certainly not the answer to these questions (although it plays a very small part) and neither is the fact that certain places register better or fairer. And it being a matter of time before the situation is the same worldwide is also false. There are clear explanations for the above. Understanding their consequences heavily influences which exit-strategy we choose/must follow (worldwide).
R0 very high
Very soon it became clear (I read it on Twitter already in January) that the R0, the reproduction factor of COVID-19, was very high. In February it showed to be around 2,25. (1,3 for regular flu). This means that when no measures are taken, 1 person could infect on average 400 others in a one-month time span.
Everywhere authorities tried to bring that R0 to below 1 as soon as possible, and they were right to do so. If they hadn’t, the number of new cases would only increase faster.
Three things stand out when we look at outbreaks that occurred up until one month ago:
- Most of them occurred between 30- and 60-degrees latitude, in a climate zone where the weather at the time was between 4 and 11 degrees and the humidity between the 3 and 6 g/kg (grams of water in 1 kilogram of air).
- There are big regional differences between countries with outbreaks. Lombardy has 20 times more deaths when comparing it to Naples and Rome. And the Netherlands, Spain and the US clearly show a similar pattern.
- Often been gatherings of large groups that infected many individuals in one go. (The superspread events). Zooming in on these gatherings shows that it were mainly gatherings where people have yelled or sung. This involves both small and large scale ecclesiastical gatherings, parties (like après-ski and carnaval) and soccer games.
Looking at last month’s development shows:
- Despite many countries located below 30 degrees latitude having been infected, very few of those places show outbreaks the size of Western Europe and New York. This doesn’t seem to relate to the quality of the taken measurements. (And don’t say that those countries are hiding their high death rates. If they had faced a severe emergency-situation then surely social media would have let the world known.)
- All East-Asian countries have control over the outbreak. This doesn’t mean there will be no small areas with high spreading infection, but these will be eliminated very quickly. To illustrate, the number of deaths per million inhabitants on the 11th of April: Japan 1, Taiwan 0,3, Singapore 1, Thailand 0,50, Malaysia 2 and Korea 4. (Both the last two countries had a big outbreak during a religious event that lasted for multiple days and had over 1.500 infections, yet they managed to completely regain control over the spread.) The province in which Wuhan is located experienced 70 deaths per 1 million citizens. But in Beijing there were only 8. This looks like Korea’s pattern. The province of Daegu had a big outbreak, and faced 60 deaths per million, whereas Seoul only had 2. (Not per million but in total).
- Many deaths are in nursing homes.
- Many cases at ships (cruises and navyships)
- Two to three weeks after lock downs show that the number of new cases stabilizes, and then drops.
Explanation
There is an explanation for all the above. Supported by studies on influenza, including experiments with animals, and research about COVID-19.
This explanation is, that the spread of this virus takes places mostly through the air in (semi) closed off spaces. More so than any other way.
Forms of infection that the media so frequently mentions, could cause an R0 of 1,1 or 1,2. Measures like social distancing and/or wearing masks are aimed at getting that rate below 1,0.
Science also tells us that when people speak, couch or sneeze they emit microdroplets (aerosols) which stay airborne for a long time, thus meeting almost all people in that space. It only takes one single individual to be infected (that doesn’t know he/she is) and you’re done.
(Unfortunately, the WHO and RIVM thought up until recently that this form of spreading didn’t happen that much.)
Scientific experiments have shown that
The effect of these aerosols is much less in well ventilated spaces.
The aerosols stay afloat for a long time in air with low humidity. They float the least at a humidity of around 6 g/kg (at 20 degrees that is a relative humidity of 45%.
Above this level of 45% the risk of getting infected increases again. However, above 80% humidity and/or 30 degrees there is no infection through air at all. (see graph below)
When we apply this information to the previously asked questions, we can answer them all.
Germany
Big outbreaks have (mainly) occurred in poorly ventilated spaces with a relative low humidity where many people gathered enthusiastically. After these so called superspread-events the spread has continued at smaller gatherings in the first two weeks of March (like church meetings, choir repetitions and parties like weddings and festivities).
The maps of the Netherlands and Germany below clearly show the relation between COVID-19’s outbreak and the distribution of Catholics in the country. The first superspread-event was carnaval. Then the infected that attended the Catholic church infected the rest of the Catholic people.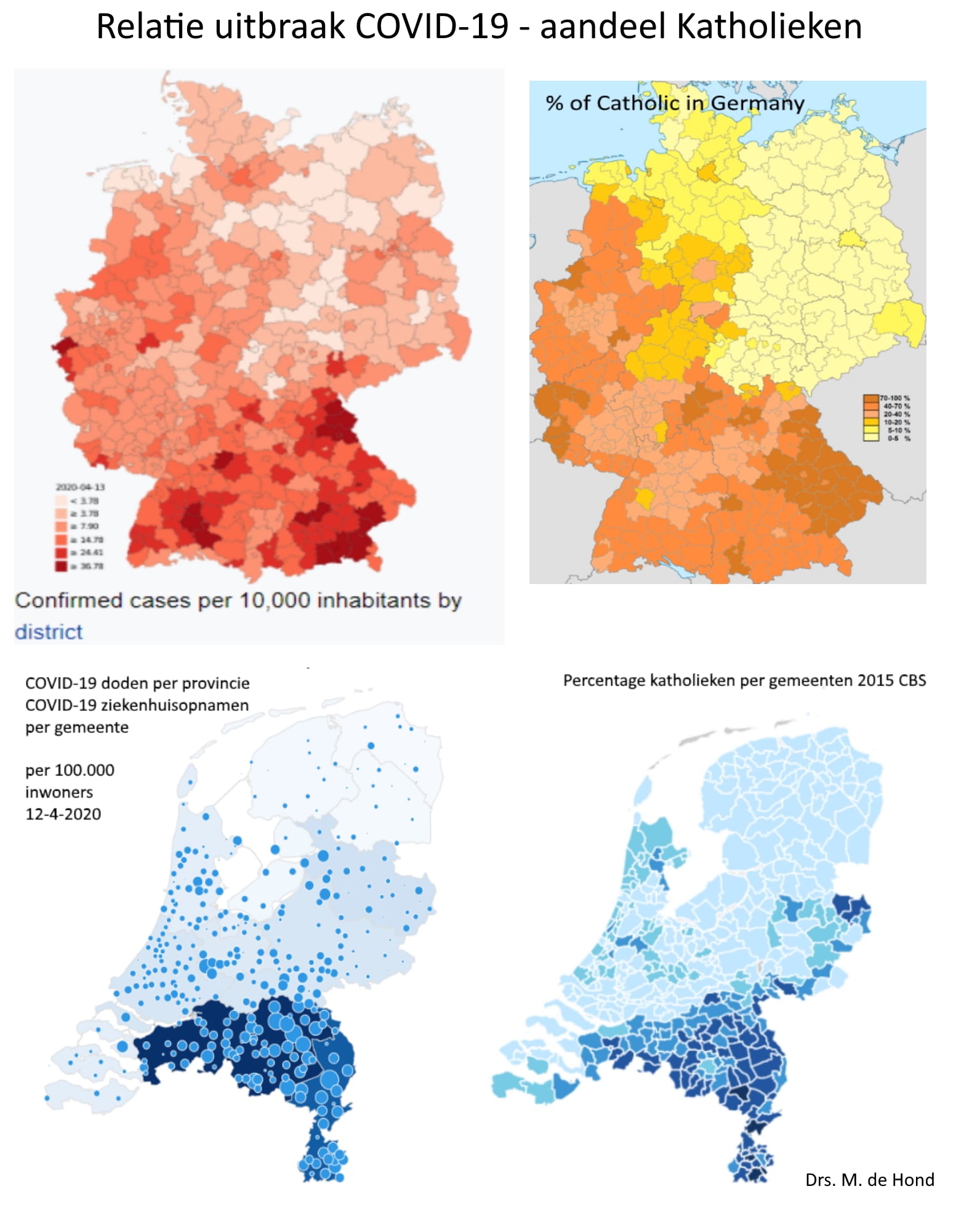
Bilble Belt
After that, thanks to “Day of Prayer of the Crops” on the 11th of March, in the Netherlands the entire Bible Belt got infected.
- Gatherings where people sung (churches, parties) and -mind- the internal air circulation, which spreads aerosols through the building, are responsible for much more victims in nursing home outbreaks than direct infection via visits or caretakers/nurses.
- The main reason East-Asia has such low death rates is because they started wearing masks very quickly (if they didn’t already). This did not only prevent infection of those wearing the masks, but it also prevented the wearers of intentionally infecting others. That’s why there haven’t been as many deaths in regions outside of the outbreak epicenters.
- The fact that refugee camps, townships and favelas didn’t have any big outbreaks is partly because people don’t live in closed spaces, often without windows so ventilation is good. Plus, the humidity helps against spreading the virus, and the temperature is often above 30 degrees. This also counts for many parts of Africa and South-Africa.
- Australia too shows outbreaks smaller than Western Europe or the US. New South Wales (where the first cases were reported even sooner than in the Netherlands) had 3 deaths per million inhabitants. (On March 21st we saw on TV in the Netherlands how many Australians went to the beach. 23 days later there is definitely no big outbreak, opposing to what the Dutch media almost explicitly predicted.)
- Few hot and humid places do show large outbreaks, Louisiana being the best example. At Mardi Gras, over a million (!) people gathered. It is not unrealistic to think that during this event tens of thousands of people got infected. The number of deaths in Louisiana, 7 weeks after Mardi Gras is now at almost 200 per million inhabitants. I think that after Mardi Gras the churches played a big role as well in further spreading the virus over there. In Georgia the number is already up to almost 40 per million.
hebbenhttps://www.maurice.nl/2020/03/27/wat-gebeurt-er-in-de-sub-tropische-gebieden-met-de-verspreiding-van-covid-19/ - Finally, German research has shown that the chance of people infection one another by touching the same surface (like supermarket trolleys, door handles, elevator buttons) is very small.
Victims
When looking at how the number of people ill or dead in the Netherlands develops approximately three weeks after the intelligent lockdown, we can first see stabilization and then a clear drop. Especially in Brabant and Limburg. (Some other provinces seem to have had new areas of fast infection due to “Biddag van het Gewas” on the 11th of March, which caused the drop in numbers to come later.)
Especially when we realize that far from a small part of the current victims in the Netherlands are in nursing institutes (I’m estimating at least half of all daily deaths), we can estimate that the rate of infection outside of these institutions has dropped significantly. This is also because since a couple of weeks there have been no gatherings of big groups of people anymore.
Taking all the above into account tells us how we can taper off the measurements and keep the risk of further spreading at a minimum. And also to succeed as a society revive our economy and social life. Like the lockdown, this can be done in a smart way too.
That’s what I’ll write about tomorrow.
You have just read: This is how the spread of COVID-19 generally takes place.







