An overview of what we currently do and do not know. Topics discussed include seasonal patterns, a comparison with the reproduction factor of influenza, mortality rates, differences in measures between countries and the necessity of strict measures including, perhaps, a full lockdown.
Lees volledig artikel: How much of an actual threat is the COVID-19 virus really?
How much of an actual threat is the COVID-19 virus really?
On this map the spread of the virus is monitored in real time. However, this only concerns the “cases” and that partly depends on how much is tested per country.
But if we look at the map, it is important to look at and understand the differences per countries/regions. And also to put these figures into perspective.
We know that in some parts of the world, outside of the (sub-)tropics, flu epidemics almost exclusively occur in winter times. The big (and crucial) question at this moment is, does the COVID-19 virus take on a similar seasonal pattern, as described in this blog I wrote.
At the moment, all government policy is aimed at slowing down the transmission of the virus from an infected on to ‘clean’ one(s). How fast this happens is called the R0-value.
The R0-value of the flu is estimated to be around 1.3, which means that someone who is infected transmits the disease to on average 1.3 other people. Consequently, when 5 people have the flu will after 5 rounds have infected 45 people.
Higher number
Right now, COVID-19’s R0-value is estimated to be well over 2, which gives a way higher number of infected people than the flu. For example, after 5 rounds of infection, there will be 300 new people with the virus, instead of 45.
Which individuals fall into a critical condition or even die is hard to say. Not everybody gets tested, and a country’s demographic structure plays a big role too. Especially the percentage of people above the age of 70, as they are more physically vulnerable. South-Korea tests many people and their results show that from those who are infected, around 1.5% dies.
Based on the information from China and South Korea, it is possible to estimate the number of people dying by age group. So the top line means that of the people over 80 who are infected, 10% die. (These figures will be updated as more information comes in worldwide. The suspicion is that as more tests are done, these figures will decrease a bit).
Zero measures
Another important question comes to mind when we think of a situation in which we would have taken zero measures to stop the spread. How many people would then fall ill and how many of them would die?
Still nobody knows the answer. This Nobelprize winner could already predict the virus’ trend in China from mid-February and his article explains it well.
He estimates that 20% of the people can get the disease. Say both his number and the South-Korean number of 1.5% are correct. Then that would mean around 0,3% of the population will die from this disease. For the Netherlands that means around 40.000 deaths. The international numbers indicate that more men than women will die and that most of the deaths will come from people older than 70 who already suffered from previous health problems. Italian research supports this.
But what if the percentage of infection and deaths appears to be higher? Even if all Dutch citizens were to be infected the percentage of deaths will be significantly lower than the 1.5% (partly because the mortality rate below 60 years is low). In that situation there could be maximum 125.000 deaths because of the virus in the Netherlands.
Update
(Update 10-4-2020: Research by Prof. Streeck shows that 15% of the population in Kreis Heinsberg is infected and that 0.37% die. Even if all Dutch people would be infected, this would mean around 60,000 deaths).
Apart from death cases there will of course also be plenty of people falling seriously ill who later suffer from chronic effects.
For many reasons it’s good to lower the R0. In China people have succeeded to bring it back to (almost) 0. South-Korea also seems to be pretty successful. Here their strategy is described in depth.
And this is the development of the number of new cases per day. The country has three times as many inhabitants as the Netherlands, there is a lot of testing and there is no lockdown.
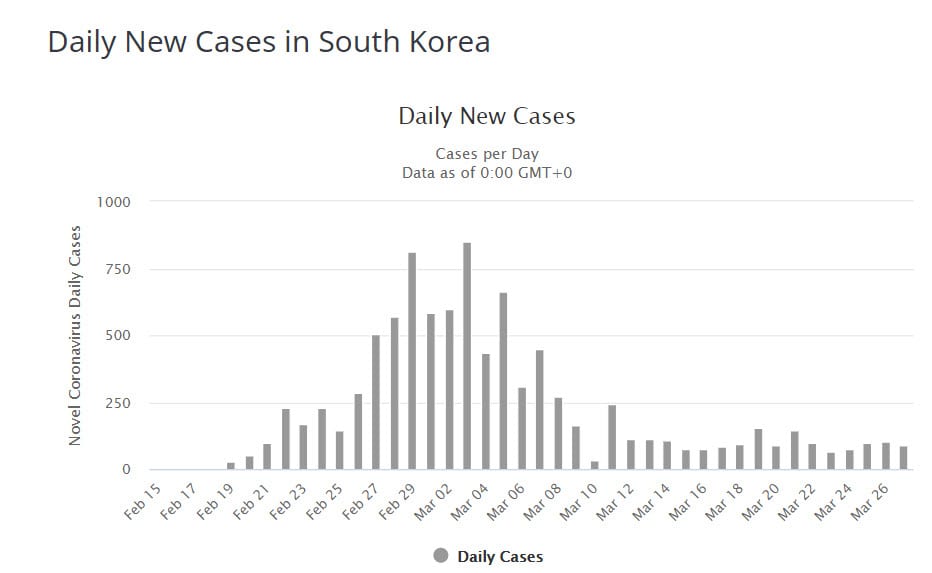
Disappear by itself
Despite their effectiveness, it is important to realize that the time these measures can be applied, even the ones from South-Korea, is finite. We hope the virus will eventually disappear by itself (like SARS did in 2003), or that we find a vaccine or good medicines. South-Korea’s policy, as well as many other countries’, will continue to aim at reducing the R0-value and keep the number of infected in their own country as low as possible. They will also ensure no outsiders, who may possibly be infected, enter their borders, or be quarantined first.
Other countries, including the Netherlands, are trying to reduce the tempo of infection (“Flatten the Curve”) to minimize the pressure on the healthcare system and enable it to take enough care of the critically ill. This spreads the infections and illnesses over a longer period of time.
COVID-19 is a vicious virus that -apart from the very ill and dead- has a big impact on a social, societal and economical level. Healthcare systems are quickly reaching their limits, worldwide the pandemic is costing billions, entrepreneurs and employees are at home and the risk of an economic crisis is rather high.
Sour apple
That each of us has to contribute to the deflection of the curve is obvious. The R0 has to go down. The sour apple is called: good hygiene, “social distancing” and maybe even a total lock down as is happening in many countries by now.
But the risks of this approach are also very high due to the direct and indirect consequences of, as it were, abruptly stopping society. I write about this in another blog: When will the cure get worse than the disease?
These 6 blogs form a coherent whole:
How great is the danger of the COVID-19 virus really? (this blog)
The influence of humidity on the spread of the COVID-19 virus
What is happening in the (sub)tropical areas with the spread of COVID-19?
How do we respond to the positive effect of a higher specific humidity?
What if the diffusion rate of COVID-19 has dropped to -near-zero?
The enormous economic and social consequences of this pandemic
You have just read: How much of an actual threat is the COVID-19 virus really?







