If your tool is a hammer, then every problem looks like a nail. This article discusses evidence that weather patterns clearly affect the spread of the virus, and why this cannot be explained by droplet transmission alone. Insisting that upticks in cases are caused by a failure to keep enough distance, the WHO and its experts are doing more harm than good.
Lees volledig artikel: The carpenters of the WHO
The carpenters of the WHO
When I hear the experts of the WHO/RIVM/OMT, I always think of Maslow (1966) who said that if your only tool is a hammer, then every problem looks like a nail.
According to the WHO (and the Dutch CDC and almost all virologists/epidemiologists in the media) Covid-19 is spread by larger drops. If someone coughs, sneezes or talks and you are too close (within 1, 1.5 or 2 meters, depending on which country you live in 😉) a drop can infect you. This can also be indirect, it is said, when a drop lands on a surface that you touch and which you then transfer to your eye.
Based on this, all kinds of measures have been taken to ensure that people stay as far from each other as possible, using the code word “social distancing”. If the number of new infections clearly decreases, they state that it is because people have kept that distance. If there is an increase in new infections, they say it is because people did not keep that distance.
With some small nuances this has been the line of the WHO and its loyal followers, from the beginning of this year. And if any other possible spread (such as through the air) was pointed out, it was first denied and then reluctantly acknowledged under constant pressure, but immediately trivialized.
Part of the problem
Now that there have been new outbreaks all over the world where they were not at first, or where they seemed to be under control, we see that the supporters of the WHO are behaving in accordance with Maslow’s statement about the hammer and the nail. “After the measures have been eased, we see another increase in the number of infections, people are once again coming too close. So we have to take tougher measures again: new lockdowns, tighter social distancing, etc.”
But what those experts of WHO and supporters don’t realize is that they are all, as another statement says, “not part of the solution, but part of the problem”.
Let me explain:
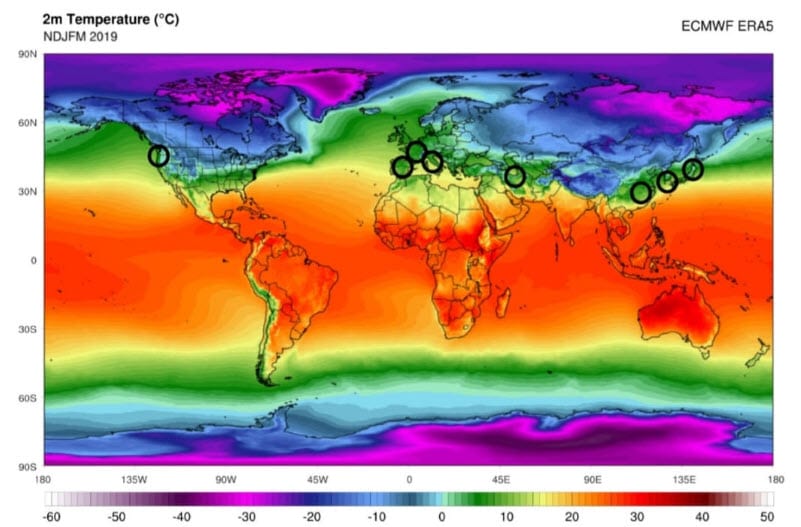
I started analyzing data on the spread of Covid-19 at the end of February – beginning of March was because I saw that the virus was really only spreading in the areas with a certain type of winter weather. This appeared to occur above 30 degrees north latitude with temperatures between 4 and 12 degrees and a specific humidity of less than 6g/kg.
When I was looking for explanations for this, I came across influenza studies over the past 15 years, which showed that people in those areas, due to those weather conditions, were more likely to stay in confined spaces and that the low humidity in those spaces meant that the influenza virus could stay in the air for a long time. I described this here at the end of March.
This is the map with the average temperatures in the world in the month of February and the circles with the big outbreaks around March 1st.
This led me to an important conclusion, which can be drawn even more emphatically today than back then.
There are very clear regional patterns, that indicated that the spread of the virus is clearly linked to the weather in those regions.
Look at the current situation in many countries in Western and Northern Europe. We now see very little hospitalizations or deaths and low numbers of new cases. Could that really be because the population in all those countries is behaving so neatly in accordance with WHO regulations? Why is there nowhere in Western Europe a kind of Floridian or Texan outbreak? Why do we see clear increases in all Balkan states? And why are there presently major outbreaks in India and South Africa, while nothing happened three months ago?
Because people were behaving according to the WHO regulations and now they aren’t?
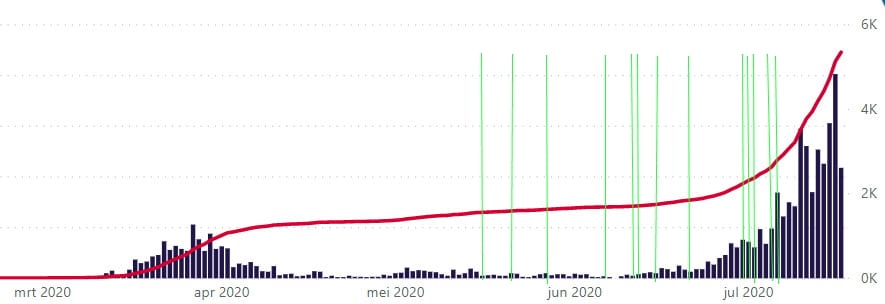
Look at Melbourne, where there has been a marked increase in new cases since early July. Is it because, from the beginning of July, people no longer adhered to WHO instructions on social distancing, whereas they did in the two months before?
Recognize that in Melbourne in June, the weather was already below 6g/kg for a few days, and from 27 June onwards it was below 6g/kg for a few days in a row (green are the days where in the afternoon or evening the humidity outside was below 6g/kg).
If you hear the WHO and related experts, you would say so. Because we have to keep our distance from each other, otherwise we will be infected by the drops that fall to the ground within 1 meter of the patient. But that’s of a logic defying simplicity.
The basic patterns in the world
When you look around the world, there are a number of clear patterns to recognize. These are, by the way, very similar to the annual spread of influenza around the world:
In areas above 30 degrees N and below 30 degrees ZB, the virus strikes between late autumn and sometime in spring. This is clearly described in this study from March. That’s why we’re now seeing the sharp rise in Melbourne and also in South Africa, where it’s been quite cold in the Johannesburg region for some time now.
In the (sub-)tropical areas the virus, just like influenza, emerges during the rainy periods. In Brazil that period is between March and July (and then migrates from North to South). And in India it is during monsoon (from June to September, migrating from West to East). You have many areas in South America that have a rainy season twice a year and there you also clearly see the virus breaking out during those periods.
Near the equator there are less clearly defined rain periods. But also there we see clear relationships with heavy rain showers (as was the case in Manous and Guyaquil in March).
In addition, there is another pattern which is more or less independent of low temperatures and rain and which was not so conspicuous in the case of influenza. There is a clear connection between outbreaks in regions where the temperature has risen sharply and air conditioning is widely used. You can see this in the southern states of the US, but you can also see it very well in the Balkan states. Where the clear increase in cases came shortly after temperatures rose to around 30 degrees C. You see it in the Middle East (Israel, Iraq, Iran). Plus the outbreaks in Saudi Arabia also seem to be related to that. In Pakistan, it is reported that the outbreaks occur mainly amongst rich people.
Throw those blinders off; it’s the aerosols
And that brings us to the heart of why I say that the WHO’s approach defies logic.
If the spread of the virus is overwhelmingly due to infections through droplets that can hit you and infect you if you are too close to an infected person, how can you explain patterns where countries in the same region and with the same climate show the same trends? Because the population of – let’s say – the Netherlands, Austria and France behave identically at the same time?
Of course they don’t. And actually, the WHO and its experts have been working hard for years to explain why the spread patterns of the flu across the earth are the way they are.
This comes from a presentation by one of the WHO doctors in 2014.
Too close
In the rest of the presentation, which is excellent initself, one tries in many ways to find an explanation: “people are too close together”, “it has to do with the school holidays”, etc. etc. But they themselves come to the conclusion that in the end it does not offer an explanation for the observed patterns in the different parts of the world.
And both with influenza and now with Covid-19, there is only one logical conclusion to draw from the inability to interpret those patterns then and now; a gigantic basic error is being made: Neither influenza nor Covid-19 spread primarily through those larger droplets. In both cases the virus spreads primarily through the air.
If you take the latter as an explanation, you can suddenly understand why in countries in the same region and climate the patterns are very similar. And then all of a sudden you can explain why it has now started to break out in Melbourne at the very beginning of July and that in the southern states of the US it is now much worse than a few months ago and in New York exactly the other way around. And you can also give a rational explanation for that years of searching for the patterns of the flu waves.
Droplets
Weather conditions have little influence on the behavior of larger droplets, which can hit a non-infected person within a radius of 1.5 meters, in nose, mouth or eye, so that they become infected.
However, the weather conditions do have a major influence on the behavior of the smallest drops. Namely, whether or not they float for a long time.
In the winters above 30 degrees North and below 30 degrees South people are more often indoors without good ventilation. When the humidity drops below 6 g/kg, the smallest drops remain airborne for a long time and can be inhaled by those present. (And studies since the 1950s have shown that you get much worse symptoms when a virus that focuses on the lower respiratory tract can nestle directly in your lungs). Wells already showed this in 1955. In the meantime I have seen many more studies that claim this since those years. (1)(2)(3). And – very spicy – also this study of Dr. Peter Teunis of the RIVM from 2010.
In (sub-) tropical areas the unique situation during a rainstorm is, that around every house a “curtain of water” hangs, as it were, that plays the same role as walls and windows in winter above 30 degrees. There is no exchange of air between inside and outside the house. The water stops that.
Poor ventilation
And when people in very warm rooms turn on the air conditioning, you also create conditions with poor ventilation with the outside air, a lower temperature and low humidity, which are beneficial for the aerosoles to stay in the air longer.
I’m not going to present the evidence again of the major role that aerosols play in both flu and Covid-19. I’ve done it in several articles, like this one and this one and this one.
Two important sources I recommend you read, if I can’t convince you.
This one by Prof. Jimenez. And this one from Dr. Fluxman.
Prof. Jimenez has also made this review.
The beauty of this overview by Prof. Jiminez is also, that he exposes so nicely how the carpenters with only a hammer, bend over backwards to be able to explain the bigger superspread events: “They have been drinking coffee together” (Prof. Van Dissel). Or “outside you’re getting it too, just look at the Atalanta Bergamo- Valencia match” (OMT and Premier Rutte), for the sake of convenience forgetting that the spectators had to travel 50 km because the race was in Milan.
An important point of the argument of those who say that Covid-19 does not travel by air I would like to highlight briefly. Because there they use a way of reasoning that is devoid of any logic:
One states (and we always see and hear this argumentation): Measles is aerogenic and has a reproduction factor between 12 and 20. Covid-19 has a reproduction factor of 2.5, which indicates that it cannot be aerogenic then.
Two of the many arguments against this:
- Not every virus that goes through the air is equally contagious. Maybe the inhalation of 10 virusparticles of measles makes you sick already and maybe you will need 500 virusparticles of Covid-19. This has major consequences for the reproduction factor. But it doesn’t say anything about whether or not they are aerogenic.
- Adams and Cowling state that 10% of the infected infect 80% of the new ones. Calculating that, means that at that 10% there’s an R0 of 20… I’ve worked that out here. That would mean, in accordance with the proposition that apparently a high reproduction factor indicates aerogenic contamination, with that argument with respect to measles compared to Covid-19 one implicitly acknowledges that Covid-19 does go via the air.
But if you only have a hammer at your disposal…..
…then you also use arguments, which defy all logic, not to have to use another tool.
Willing to admit
Yes, our carpenters are now willing to admit that aerosoles can play a role, but a (very) small role, they say. More and more virologists and epidemiologists however, indicate that this role is/can be greater than that of large drops, but they are still ignored by the mainstream.
Realize that so far the evidence for ALL three ways in which you could be infected by Covid-19 is at most circumstantial. Aerosoles, large droplets, or through surfaces. But if you look at the dispersal patterns and the overviews of Jimenez and Fluxman and you still dare to claim that the role of aerosols is at most small, then you not only show that your blinders are shut, but also that they are attached to the part of the brain that serves logical thinking.
It is debatable whether the importance of aerosols is 60%, 70%, 80%, 90% or 100%. I think I can show that it is somewhere between 90% and 100%. I do this partly on the basis of this study and here I will elaborate further
But whichever of these values it is, it is more than clear to me, that because the WHO/RIVM/OMT have chosen the line that “Covid-19 spreads (almost) only through “direct contact” and that they have not fundamentally changed that position on the basis of advancing insight, they are responsible for the increases in the number of victims worldwide. But also that politicians have introduced indiscriminate measures such as social distancing, which cause great damage to the economy, society (and public health).
Deltaplan Ventilation
Plus, thanks to those carpenters, we don’t focus on what can minimize the outbreaks in our region next fall and winter. (e.g. ensuring that ventilation is in order in all enclosed spaces, as indicated in the DeltaPlan Ventilation).
It is about time that politicians, administrators, journalists and citizens recognize that this inflexibility of WHO and CDC’s thinking is doing the world more harm than good.
You have just read: The carpenters of the WHO.
Volg Maurice de Hond op Twitter | Facebook | LinkedIn | YouTube.