The WHO's website indicates a social distance of 1 metre. But in the Netherlands, we are told to keep 1.5 metres distance. What is the added value of those additional 50 centimetres in terms of public health, what are the economic and social costs, and where did the 1.5 metres come from?
Lees volledig artikel: The blind spot with huge consequences
The blind spot with huge consequences
Introduction
It is important to know where that 1.5 meter which we hear so often, actually comes from. And how logical that rule is in the light of the recent studies, which have been carried out on Covid-19.
First of all, the WHO indicates on its website, that a distance of 1 meter should be maintained. But where does this distance of 1.5 metres actually come from?
In the literature on influenza it is stated that the transmission of that virus is mainly via droplets and direct contact. To a much lesser extent, this is indirectly via aerosols. These are tiny droplets that float through the air.
This diagram by Dr. Walter Hugentobler makes that very clear.
The Dutch RIVM (and all prominent virologists in the Netherlands) echo that the spread of Corona-19 happens via direct contact and if you stay at 1.5 meters distance there is very little risk. According to Prof. van Dissel of the RIVM, the impact of alternative transmission methods is very small.
From that perspective, keeping a distance is a good strategy. But how certain is it that the direct transmission of the Coronavirus within a radius of 1.5 metres of an infected person is indeed the prominent method of transmission?
The inexplicable seasonal patterns of influenza
Influenza has been studied a lot over the past 80 years. But if you look at those studies, there still appears to be a lot of uncertainty about how the transmission of the virus really takes place.
These are studies from which it can be determined how much we don’t know yet. (1), (2)
In 2014 there was a big congress in Dubai on infectious diseases. A doctor associated with the WHO gave a presentation on the search for an explanation for the differences in seasonal patterns in countries below 30 degrees North latitude.
You can tell when you read that presentation that they have absolutely not figured it out yet. It is best indicated with the text of this sheet.
All kinds of possible explanations come along in that report (slide 14 et seq.), but the author always observes that it is not a conclusive explanation for the differences in the patterns that exist. (Really recommendable to read).
But if that can’t be made appropriate, how can we be sure that the spread of the influenza virus is predominantly via direct contact forms within 1.5 meters of each other? That doesn’t really make sense.
With what we now know from scientific research into the spread of Covid-19, there are even more illogical matters.
Just 5 questions:
- There are various studies that show that the contamination takes place much more indoors than outdoors. A score of 1 out of 350 is reported in China and 1 out of 20 in Japan. In his research in Heinsburg, Prof. Streeck found that the vast majority of the infections had also taken place indoors.
So the first logical question is: if direct transmission within 1.5 metres between two people is so dominant in the infection of others, why doesn’t it happen outside to about the same extent as inside? After all, we also meet many more strangers outside than inside, so that should lead to many more infections.
- At least four studies by Covid-19 show that housemates of a patient are much less infected than you would expect.(1) (2) (3) (4). In these four studies we see percentages between 5% and 35%. So the vast majority of household members were not infected. But that’s actually completely illogical. After all, within a household the 1.5 meter distance will have been observed much less, especially when it was not yet known that the patient’s symptoms were the result of a Covid-19 infection.
- On March 10, a choir rehearsal of 60 men took place near Seattle. They kept to the 1.5 meters, did not touch each other and used disinfectants. Three weeks later, 75% were infected, some were dead. Similar figures, which we also see in a choir in Amsterdam. Also 75% sick and some dead. But they didn’t hold 1.5 meters.
During Carnival
Prof Streeck’s research in Heinsberg showed that those who had been infected during the carnival meeting had become more seriously ill than those who had contracted the virus at home.
But how is that possible? How is it possible that at superspreading events a significantly higher percentage is infected than at home and that they are even sicker (16% of the infections without symptoms, 36% at home)? Is this compatible with the view that the vast majority of transmission occurs via direct 1-to-1 contact within 1.5 metres?
It gets even weirder when we also know that a large proportion of the infections occurred at superspread events before the lockdowns.
- A lot of people have been infected on naval and cruise ships. This also seems to be the case with quite a few care institutions. Could that really be because all those Navy people came within one and a half metres of an infected person? Or is there another reason?
- We repeatedly see footage of poor countries in Africa and refugee camps on television. Also how it goes in India. People who live shack by shanty and shanty by shanty. Even keeping a distance of 50 centimeters would be difficult there. For two months it’s been threateningly said “if it’s going to erupt here, it’s going to be a disaster…” . But that disaster didn’t happen. Not on Lesvos, not in Africa. In India there are now 2,000 deaths out of a population of more than 1.3 billion.
Observations
So these are already 5 different kinds of observations, so you can question the proposition, that the contamination mainly occurs through direct transmission within 1.5 meters. Together with the lack of explanation of seasonal flu patterns, there can only be one logical explanation.
“Influenza and COVID-19 transmission does not occur primarily through direct contact within 1.5 metres between one infected person and another”.
So what’s another logical explanation?
But how does it go? Based on recent studies, this is my hypothesis:
“The transmission of influenza and COVID-19 is almost entirely via aerosols. You breathe them in and with that the virus enters your body. You have to be exposed to it for a certain period of time, because otherwise you won’t be infected/not sick of it”.
This is an extensive article by Prof. Shelley Miller, which describes the aerosols well.
Let’s revisit the 5 questions and assume that the hypothesis is true:
- Because aerosols dissipate in the open air and do not stay in one place, people are almost never infected outside.
- Even if you have a patient at home, it does not have to be the case that the rest of the members of the household are infected by aerosols long enough. It may be due to ventilation and humidity in the house, or that one does not stay with the patient long enough and that the patient emits few aerosols.
- In superspreading events, you spend 2 to 4 hours in an enclosed space with the aerosols of an infected person. At home, there is usually much less time in a row or there is ventilation. So that’s why more people get sick at these events.
- Through internal ventilation systems, aerosols are spread over rooms and stay there for a long time. As a result, so many people present on ships and in care institutions become infected.
- In refugee camps, in Africa and India, people’s houses/tents are such that natural ventilation always takes place. Even if aerosols are ejected by an infected person, they do not remain there long enough to infect someone. That’s why we see so few infections there.
So this new hypothesis provides satisfactory answers to each of these five questions.
Seasonal patterns
It would be marvelous if the large and year-long search by virologists and epidemiologists for an explanation of the seasonal patterns of influenza would also lead to results. Yet another proof that they were looking for this and found no explanation. This can be found in a paper from 2016.
So let’s see if with this hypothesis we can find an explanation for the start of an influenza epidemic in those areas. And I can already tell you, it’s been found.
So the hypothesis is, “you’ll be infected by aerosols, which will stay with you for a long time and breathe in enough to make you sick.”
- Infected north of the 30th parallel:
When the humidity is low, the aerosols remain in a poorly ventilated room for a long time. This condition only occurs in autumn or winter. This is when the flu epidemic occurs.
- In the rest of the world:
The humidity level is too high for an aerosol to stay indoors for long.
(Air conditioning is unfavorable, but if that happens in rooms where only one’s own family is present, it doesn’t lead to major outbreaks).
We see many different patterns of that flu outbreak:
– This study in India shows that the flu wave in Srinagar, in the north of the country, is only in winter (as is the case with us). There in winter the weather was about the same as in the Netherlands. In the much more southern Delhi was the flu wave during the monsoon (between July and September).
In that same study from 2014 is a list of countries below 30 degrees North latitude with different patterns of the flu. And in all countries, except near the equator, we see that the flu wave is there during the rainy season.
– But close to the equator we don’t see a clear pattern. Malaysia is mentioned as an example (also near the equator) and if one counts several years together, the picture becomes very diffuse.
How does the above fit into the hypothesis about the large role of the aerosols?
Manaus offers the explanation
I found that explanation in Manaus.
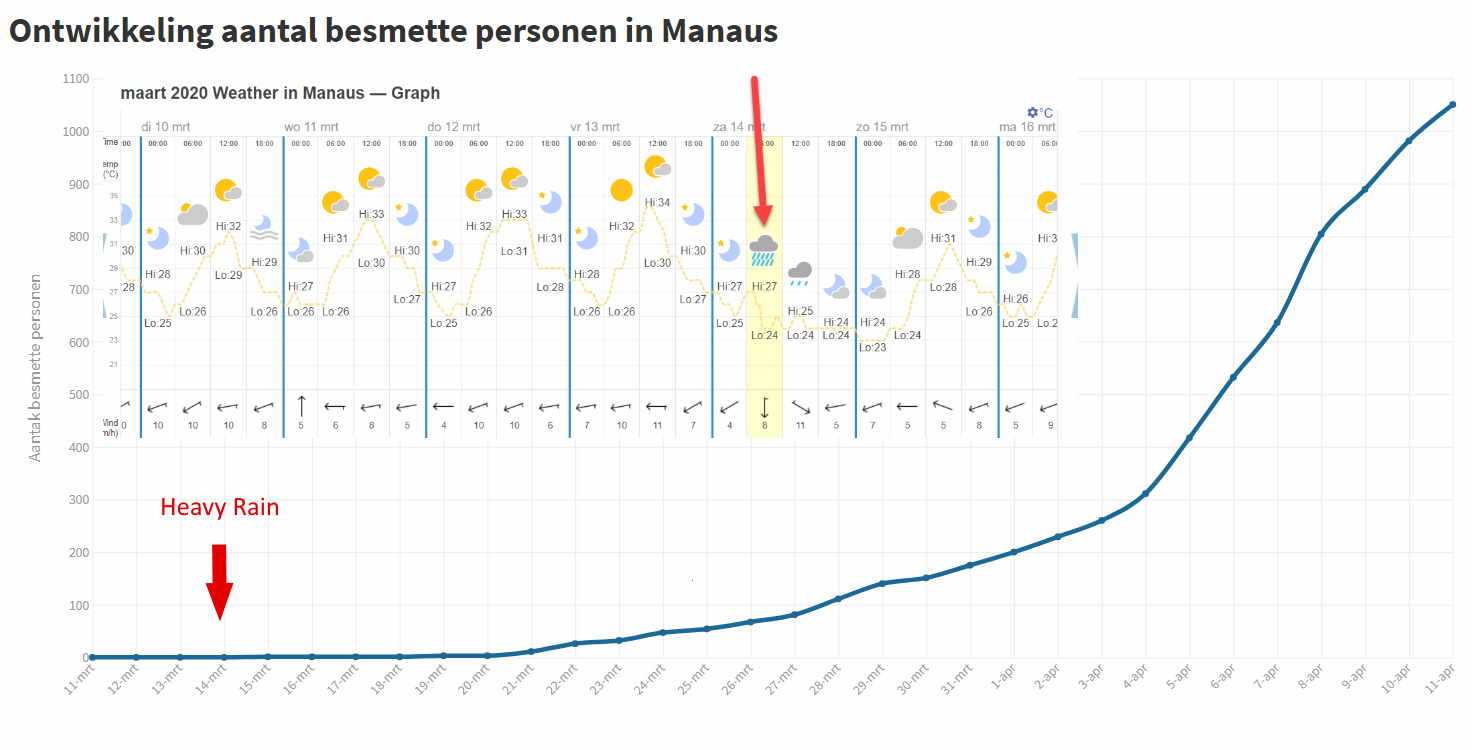
There are the daily figures for COVID-19 infections. Around March 19 the outbreak started. So something must have happened between 12 and 15 March. But what?
I found no major events. But something else. The graph below shows it. On Saturday morning, March 14, there were “heavy rains”:
From my experiences in Cuba with my in-laws, I know what happened. In the house (where there are no glass windows and the door is almost always open) live about 20 people. Sometimes you are with 8 people, sometimes with 4, sometimes with 12. People often live outside. And inside they try to keep a cool head by means of natural ventilation of the air, where everything is open. Plus some fans. Possible aerosols are driven out of the house so quickly and disappear. If they don’t precipitate quickly because of the high humidity.
Until it starts raining and storms and everyone flees into the house. The doors and windows still remain open. So still good ventilation.
But that’s not the case with such a heavy downpour. And I’ve heard that statement from an expert in that field.
That’s how he described it:
“In a rainstorm, an additional resistance will be created for air flowing in or out through an open window. So ventilation will become more difficult and this will get worse with more rain. The air has to go straight through the falling rain drops and this costs pressure drop, pressure of the air in front of and behind the rain screen”.
So when it rains hard there’s like a wall of water around the house. But there is more, and that seems to be the most important component. And that’s thunder. I remember very well how we used to unplug the TV and radio at home when there was a thunderstorm. Apparently that’s still wise. I certainly understand that poor people still do, because they are afraid that their device will break down (or a fire will break out).
So when it rains hard and it thunderstorms, in those countries they unplug the fan(s) they have. So that’s the only moment in those countries that the air indoors more or less stays still. The rainstorm closes off the escape of the air to the outside. And turning off the fan(s) ensures that the air remains fairly still in the house.
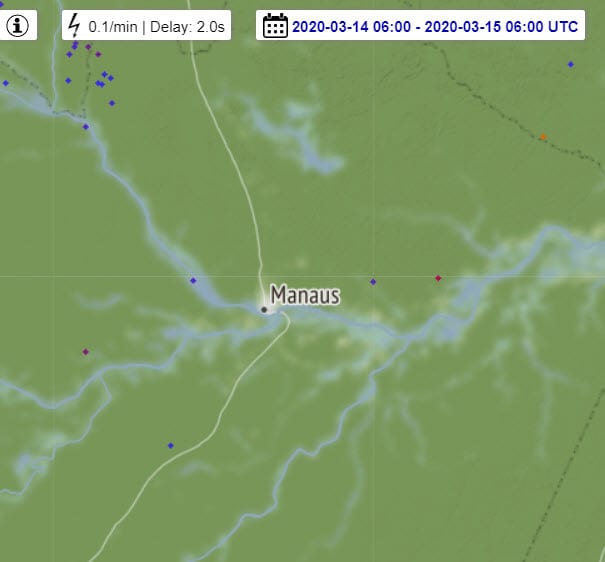
There is also an archive from the website where thunderstorms around the world are recorded. And if you go and look at Manaus it hasn’t been there for days in that period, but on the morning of March 14th.
Airflows
The air in the house cannot flow through and there are no airflows in the house. If there is a person within the household who was already infected, that person can easily infect a large part of the 15 to 20 family members.
So these are the “distributed superspreading events” of the tropical regions. And from the information I got from Manaus, it appeared that after that there were a few more similar weather conditions and each time after that there was an increase in the number of victims.
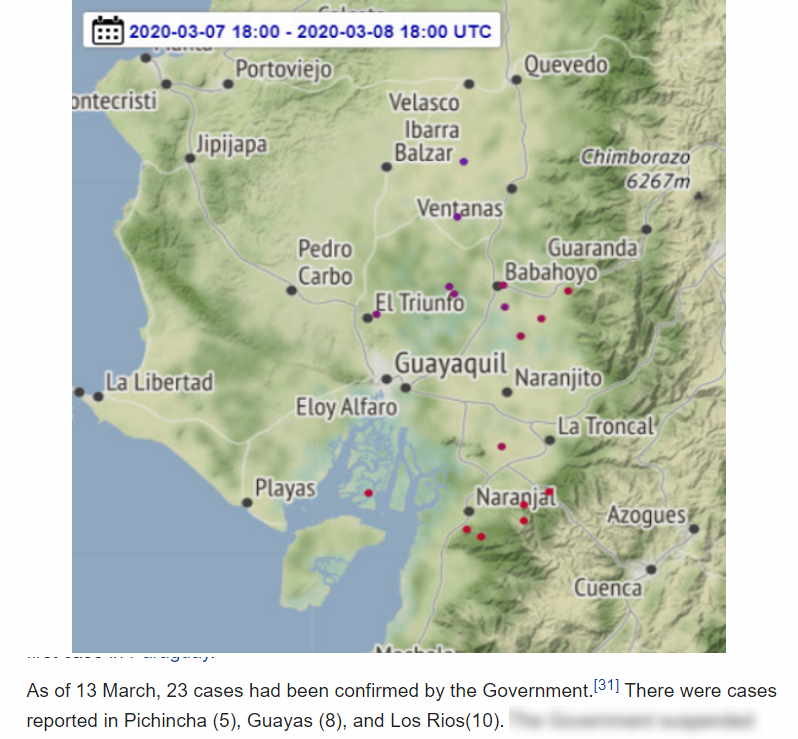
Also in Guayaquil in Ecuador something similar was noticeable. There was a thunderstorm on the morning of Saturday 8 March. And below that, in Wikipedia, we read about the new infections in Ecuador (Los Rios is located north of Guyaquil and it had also ignited there):
Thunderstorm
Another possible relationship with the thunderstorm could be what I came across here. Prof. Galembeck has done research on the electrical charge of water droplets. He found that during a thunderstorm the electrical charge in the air changes. This could be another explanation for the fact that the aerosols, which normally do not float at high humidity, show a different behaviour during a thunderstorm and remain in the air. This is a paper about his research.
Which of the two explanations is the correct one needs further investigation, but it is obvious that this thunderstorm was the starting point of a super-preadevent in Manous and Guayaquit.
Therefore one could not see a pattern at the flu waves in the areas near the equator! If you look at the averages in a few years time, you don’t see the specific moments that triggered the outbreaks. Because maybe a year before, it didn’t thunderstorm on March 14th, but on March 28th or March 2nd!
And with this explanation you can suddenly explain the differences in the patterns of the flu waves in the tropical areas. The outbreak of flu and Covid-19 occurs when it rains heavily and thunderstorms…That’s the only moment that in those areas there is no air flow in the houses and also no fresh air from outside, because “the rain screen” blocks that fresh air as it were.
In conclusion: this hypothesis about infecting someone else with aerosols is much more robust than the one that the WHO and others have been working with for years, that it is almost only within 1.5 meters. A hypothesis that does answer the 5 questions asked above and also provides an elegant and complete explanation for the long sought-after holy grail of flu research.
The major consequences
This would show that the one and a half meters is much less important than how the aerosols move through the room and whether or not they can infect people. And that has major consequences for the approach to prevent contaminations.
If the WHO (and the CDC’s) do not take this information into account quickly, this could have major consequences. If the WHO indications are (partly) based on the wrong assumptions, this will lead to many more deaths worldwide and much more damage to the economy than is necessary.
Not only is the one and a half meter society nonsensical if it is mainly the aerosols that can cause problems indoors. Combating them is much simpler and the economic and social restrictions are much less drastic.
And what protection do mudguards provide if it is mainly the aerosols floating in the air that cause the contamination?
But in terms of human lives, these indications can also lead to major disasters. Take India. There’s not much going on there right now. But in a large part of India, the rainy season will start in two months’ time. And if you don’t know the risk indoors by then, there could be a lot of casualties. While the best advice for them is to take care of air circulation (via a ventilator or otherwise) when it rains heavily (and thunderstorms).
Big question
The big question is whether all those people who thought for so long that the contamination came almost exclusively from direct contact are now prepared to recognise that a dominant role of aerosols gives much better answers to the search for seasonal patterns and the results of the most recent studies.
But hopefully there are enough people in the medical world who are willing to face facts and logic and then do everything in their power to come up with the right approaches. Fortunately, this is already a website of a group of professors and doctors who call on the WHO to measure aerosols and humidity in their policy advice.
It will save a lot of people’s lives worldwide and it can help the economy and society all over the world to return to normal faster if WHO and the CDC’s take all this seriously.
The blind spot with huge consequences.