Final proof – Humidity slows or accelerates spread of virus We are currently working with a group of scientists to produce a paper on the findings of our research into the relationship between the weather and the rate of spread of the COVID-19 virus. However, the results are so interesting that I am already giving […]
Lees volledig artikel: Final proof – Humidity slows or accelerates spread of virus
Final proof – Humidity slows or accelerates spread of virus
We are currently working with a group of scientists to produce a paper on the findings of our research into the relationship between the weather and the rate of spread of the COVID-19 virus.
However, the results are so interesting that I am already giving a sneak preview of our findings. In 69 regions we searched for a numerical relationship between the number of deaths caused by the virus and the weather in the preceding period. Below is a brief report of the results.
The input for the analysis
- 69 regions have been used for this analysis: 18 regions in Italy, 50 American States and the Netherlands in total. The total population is 403 million.
- In order to be able to compare regions, we started counting from the day the 10th COVID-19 infection was registered in those regions.
- Per day we took the number of deaths as an indication of the number of infections in the area from about 3 weeks before. To exclude coincidence per day, we took the moving average of 3 days per day. This was divided by the number of inhabitants per region. This is the number of deaths per 1 million inhabitants.
- For each location the weather information per day was retrieved between 1 February and 31 March 2020. This concerned the weather station closest to the largest city in the region. For each station the temperature was taken in Celsius, the relative humidity in percentage and the specific humidity in grams of water per kilogram of air, at a time as close as possible to 14 hours.
- For each region, the values below were determined daily from 28 days to 8 days prior to day 1:
- The average
- temperature
- relative humidity
- specific humidity
- The number of days the temperature was below 0 degrees.
- The number of days the specific humidity was between 3 and 6 g/kg.
This information was analysed with a Random Forest analysis followed by various CHAID analyses. The latter is a statistical analysis in which the interaction between variables is determined by means of a tree analysis. The analysis established the relationship between the average mortality rate per day (counting from day 1) and 10 weather variables (5 with averages of 3 weeks and 5 with averages of 4 weeks).
And the results
So two types of analysis have been carried out:
- On different days after day 1, the CHAID analysis was carried out per region. The relationship between 10 weather variables and the number of deaths in the 69 regions concerned was examined.
- It was examined how many days it took to reach 0.75 deaths per million inhabitants in a region.
In principle, each of the 10 variables (5 with averages of 3 weeks and 5 with averages of 4 weeks) had an equal chance of ending up as the most important determining variable via the analysis. Practice showed that the average temperature hardly played a role during that period. The specific humidity was always the variable that came out as the most determinant!
Analysis A. The average number of deaths per million inhabitants
This is the result of this CHAID analysis after 10 days. (Those after 15, 20 and 25 days corresponded well with this).
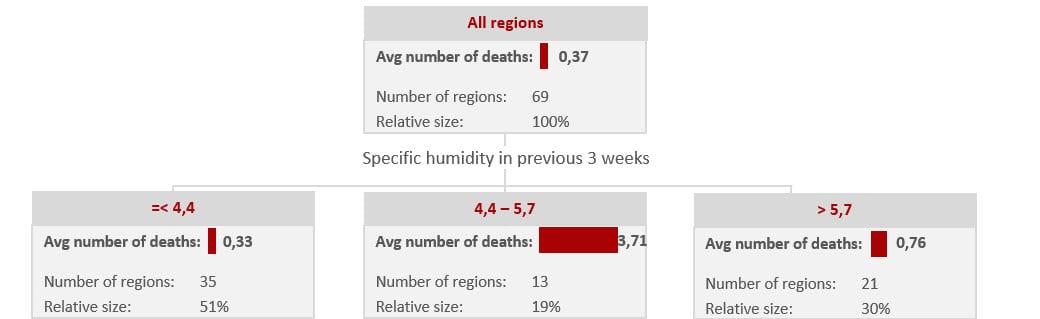
So after 10 days the average number of deaths per inhabitant in the 69 areas was 0.37.
The CHAID analysis indicated that the correlation with specific humidity was strongest, so after 10 days the average number of deaths per inhabitant was 0.37 in the 69 areas.
Number of deaths
If the specific humidity was below 4.4 g/kg in the three-week period, the average number of deaths was 0.33. The CHAID analysis indicated that the correlation with specific humidity was strongest. If the specific humidity was between 4.4 and 5.7, the average number of deaths was 3.71. At a specific humidity of more than 5.7, the number of fatalities fell to 0.76.
This is in line with M.M. Sajadi e.o.’s finding of 4 March 2020 that all major outbreaks (e.g. in Wohun, Tehran, Madrid, Bergamo and Seattle) were in a zone between 30 and 50 North latitudes, with temperatures generally between 5 and 11 degrees and specific humidity between 3 and 6 g/kg.
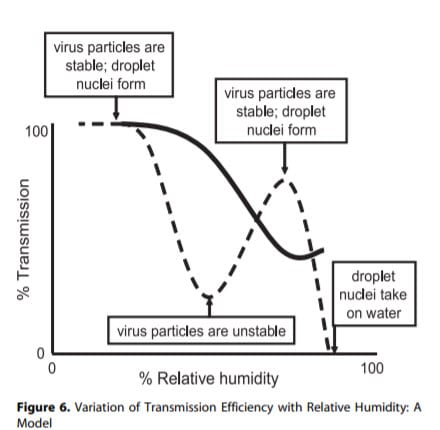
It also resembles this picture from animal studies on the spread of the influenza virus. Look at the dotted line. In the middle (which equals 6 g/kg) it has also been found in those experiments that the transmission of the virus is then smallest. So this corresponds well with the findings of our CHAID analysis.
Analysis B: How many days it took until 1 death per 1 million inhabitants was reached.
This method of analysis also provides the same picture. The speed of reaching this number of deaths has a clear relation with the specific humidity in the 3 weeks before.
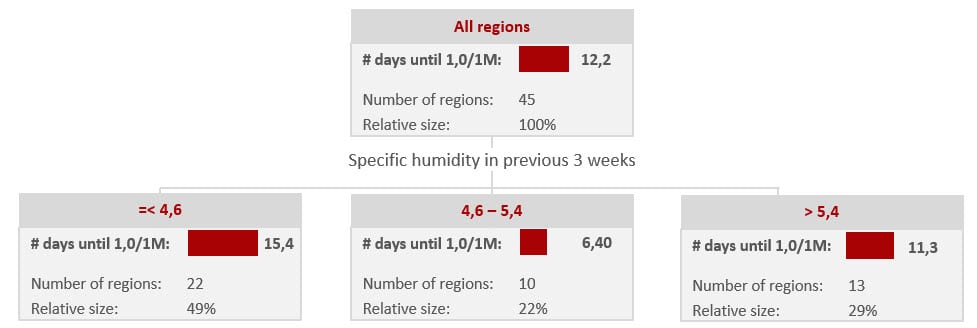
In the 45 areas where 1 death per million inhabitants was reached, it took an average of 12.2 days to reach it.
If the specific humidity in those 3 weeks before had been below 4.6 g/kg on average, it would have taken 15.4 days. If the specific humidity had been between 4.6 and 5.4, the 1 million deaths would have been reached in 6.4 days. Twice as fast! At a specific humidity above 5.4 it took an average of 11 days.
These results support the hypothesis that if the specific humidity is between 4.5 and 5.5 g/kg, the spread of the COVID-19 virus is significantly faster than if the specific humidity is higher or lower.
What does this mean for the policy?
This information must play an important role in strategies to slow down the spread of the virus.
The amount of water in the air can both help and counteract the policy to slow down the spread. This video from the president of the association of Japanese virologists, clearly shows what can happen indoors through micro-droplets, i.e. infecting everyone present in the room.
Indoors (certainly also shops, offices, hospitals, nursing homes and schools) provide the humidity of 6 to 7 g/kg. Here is the conversion calculator from relative, to specific humidity (and good ventilation).
And adjust your measures within your intelligent exit strategy if the weather outside is “unfavourable” or “favourable”. Something like happening with hay fever.
(Incidentally, research into the effect of outdoor humidity should also be carried out as soon as possible. My estimation is that the effect of contamination via micro-droplets outdoors is minimal, because those droplets then rise. But that would have to be demonstrated experimentally).
Thanks to Irma Doze (Business Economics) and Ramona Boes (Applied Mathematics) of No Ties-AnalitiQs.
You have just read: Final proof – Humidity slows or accelerates spread of virus.