Prof. Streeck's research in the heavily impacted Heinsberg/Gangelt area just across the German border, is the most complete randomized study I've seen so far. Unfortunately, the Netherlands doesn't seem intent on following this example and/or learning from this type of research. That is why I will give you an overview of its main conclusions.
Lees volledig artikel: Interesting research figures from Prof. Streeck from Gangelt
Interesting research figures from Prof. Streeck from Gangelt
Prof. Streeck, who researched Covid-19 spread in the severely affected Heinsberg/Gangelt area (Germany) was on the ZDF News cast last night. The interesting paper of his research in Gangelt (just across the border near the Dutch city of Sittard) has just been published. It paints an excellent picture of what happened there after a superspreading event on 15 February 2020. Moreover, it is characteristic of what happens in a community after such an event with a major outbreak.
In the community of over 12,000 people, a sample of 919 people from 405 households was taken. A questionnaire was taken, blood was taken, a sample was taken from the back of the throat and samples were taken from surfaces in the house. The most complete random survey I have seen so far. With interesting results.
Before I go into the results, this for me shocking and unfortunately significant finding. Around the 15th of February it was Carnival, which turned out to be a superspreading event. When on February 28th it was realized that a lot of people were infected in Gangelt, a complete shutdown took place. Schools closed, all places where groups of people could gather, public transport stopped and a variety of other measures were taken. 1,000 partygoers went into quarantine.
Kessel
So this was on February 28th, near the Dutch border. On March 5th, a charity event with 500 people took place in Kessel, 40 kilometers from Gangelt. That was also a superspreading event, which I wrote about earlier. Shortly after, a lot of people turned out to be infected. No specific measures were taken in Kessel. Except the generic measures that were taken around March 19th for the whole of the Netherlands. No specific investigation was started in that municipality either.
At the end of March the outbreak was picked up by the regional press. The Kessel case did not reach the national media until around mid-April. On April 19th, National newscast EenVandaag brought a segment with the significant title “But why here, in this small village?”. In 6 weeks 165 people had died in that municipality. In week 13 (end of March) 5 times as many people died as the average in weeks 1 to 10.
And in the meantime, the municipality belongs to the top 5 municipalities in the Netherlands in terms of the number of infected people, hospital admissions and deaths.
So while Gangelt locked down 2 weeks after the superspreading event on February 15th, there was no intervention in Kessel. Nor that at the end of March a major research program was started in that community. What a difference of approach between the Netherlands and Germany! The qualification “well-meaning amateurs” for the approach in the Netherlands is the most positive thing you can say.
Prof. Streeck was interviewed in the ZDF newscast.
He presents his most important findings. Meanwhile I have also read his paper and this is what I think are the most important findings:
- 22% of the people who were infected didn’t notice it themselves and had no complaints.
- 0,41% of all infected people have died. This means that the IFR (Infected Fatality Rate) is calculated at a maximum of 0.52%. If this percentage were to apply to the whole of the Netherlands, the infection rate would already be somewhere between 15% and 20%.
- Streeck shows that the people who were present at the superspreading event had more symptoms and were sicker than the people who were infected elewhere (by a factor of 1.63). Those infected at that superspreading event showed no symptoms in 16% of the cases. Those who were infected elsewhere (especially in their own household) showed no symptoms in 36% of the cases. This confirms the image that patients become sicker the more exposed they are to the virus. But also that you apparently come into contact with the virus more intensively during a superspreading event (with floating aerosols) than when you are infected, for example because you live at home with an infected person.
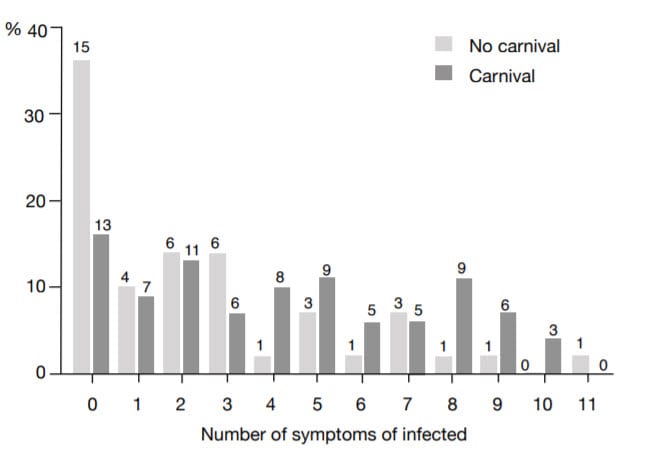
- The chance that you were infected by a family member turned out to be clearly lower than you would expect. In spite of the fact that you have been in the vicinity of an infected person a lot (and therefore have certainly not held a 1.5 meter distance). In a family of 4, you therefore have a 40% risk of being infected as well. Of that, x% shows lighter symptoms.
Major consequences
The results are in line with findings in other studies and also from what I’ve written in my blogs over the past month and a half.
Those scientific findings should have major consequences for the policy that is now being pursued in the Netherlands (and around the world). Combined with what we already knew from other studies, these are my conclusions:
- Superspreading events are the most important source for the exponential growth in the number of infected people.
- The extent to which you become infected (and ill) is significantly greater if you are infected by floating aerosols than if you are infected by a form of direct contact with an infected person.
- The chance of becoming infected if you are close to an infected person unprotected is significantly smaller than previously assumed. (If you only have a 40% chance of being infected at home by a family member, how much risk do you run on the street or in a shop if you are close to someone who is infected?)
- Stopping meetings of many people, as has actually been done worldwide, has a greater impact on the reduction of the outbreak of the virus than keeping the 1.5 meter distance.
- In combination with the fact that you have a much lower chance of infection outside than inside, any restriction you impose on people’s manners in the open air is actually nonsensical. It has virtually no effect on the extent of the spread of the virus!
- In indoor areas you do have to be more careful to be infected by aerosols, rather than directly by an infected person. Caution (e.g. by mouth protection) is wise however. 1.5 meters distance is actually much less relevant.
Smarter way
Let us hope that the RIVM and virologists in the Netherlands will also take this study quickly and then take the right measures, so that the Netherlands can quickly emerge from the lockdown in a smarter way.
Interesting research figures from Prof. Streeck from Gangelt.